(U.S. Air Force photo by Senior Airman Hailey R. Staker)
(U.S. Air Force photo by Senior Airman Hailey R. Staker)
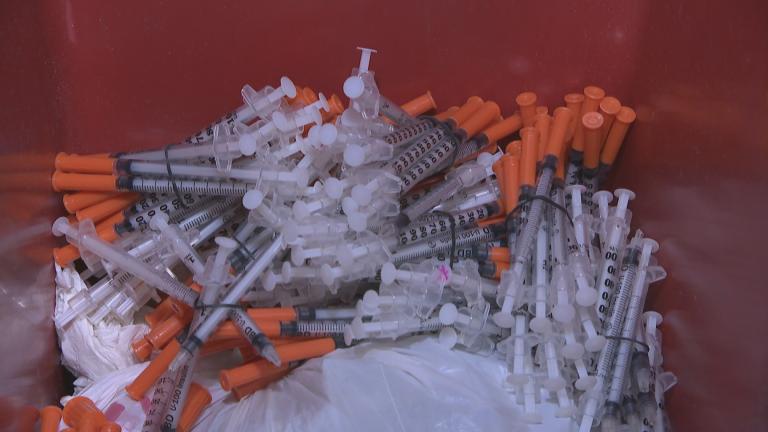
A yearslong investigation by the Washington Post offers a state-by-state snapshot of the opioid crisis, mapping the flow of prescription pain pills from manufacturers and distributors to pharmacies from 2006 to 2012.
During that seven-year span, nearly 2 billion pain pills were supplied to Illinois, according to the Post’s analysis of data maintained by the Drug Enforcement Agency, which tracks the path of every legal pain pill sold in the U.S.
“I would love to say that I was surprised, but I was not,” Illinois Attorney General Kwame Raoul said of the Post’s findings. Raoul, who was elected last November, said his office is privy to such information given ongoing investigations into opioid distributors and manufacturers.
In April, Raoul’s office filed a lawsuit against Purdue Pharma, an opioid manufacturer based in Connecticut, for allegedly using deceptive marketing practices to increase prescriptions for its painkillers. “Rest assured we’re looking at far more than just Purdue and those entities are aware of it,” Raoul said, adding the number of lawsuits his office files doesn’t reflect all the work it’s doing to address the epidemic.
His predecessor, Lisa Madigan, joined a coalition of 41 attorneys general to expand investigations into opioid manufacturers and distributors, including several of those named in the Post article.
And Raoul notes the epidemic is worse than the DEA data suggests, because “many people moved on from prescriptions to illicit drug use.”
According to the Illinois Department of Public Health, more than 4,600 Illinois residents died from an opioid overdose between 2008 and 2012.
“There is not a corner of our state that’s not impacted,” said Raoul, who earlier this week wrote a letter to Congress urging the removal of federal barriers to opioid use disorder treatments.
Efforts to curb the epidemic are ongoing in the state. Among them is the 2018 mandate that anyone who prescribes controlled substances in the state register with the Illinois Prescription Monitoring Program (PMP), which collects information on controlled substance prescriptions and allows prescribers and dispensers to access a patient’s prescription history.
Prescribers are actually required to view the PMP when considering prescribing opioids, but that can be burdensome for practitioners, according to the Illinois Department of Human Services. State law mandates that by 2021, PMP data must be directly incorporated into a patient’s electronic health record.
Illinois also loosened restrictions on its medical marijuana program, opening it up to anyone who would otherwise be prescribed an opioid.
Visual messaging and storytelling are also at play in the state, in addition to funding for research.
The Drug Enforcement Agency in February launched a digital billboard campaign warning passersby of the dangers of opioids and outlining treatment options across the Chicago area.
And last year, Cook County Sheriff Tom Dart launched a podcast about the opioid crisis. “Breaking Free: Dispatches from the Opioid Crisis” aims to expose the “devastating nature of opioid addiction,” according to the sheriff’s office. Since 2016, health officials at Cook County Jail have been providing at-risk inmates with an opioid overdose-reversing drug when they leave jail.
In July, the National Institute on Drug Abuse awarded the University of Chicago a five-year, $17 million grant to study how to reduce opioid addiction and overdoses in prisons and other justice settings.
“More than half of the people who use opioids end up in jail or some sort of correctional setting,” said UChicago infectious disease researcher Dr. John Schneider in a statement. “If we can engage the justice community around this problem, maybe we can make an impact.”
IDHS has been awarded more than $82 million across four federal grants to address the opioid crisis, including increasing public awareness of opioid-related problems and access to services and expanding the availability of medication-assisted treatment. In late 2017, IDHS launched a free hotline for people who use opioids and other substances. As of June 24, 2019, the hotline received 14,014 calls, according to IDHS.
Mental health services are also part of the conversation, including telehealth services. Late last month, Chicago-based Regroup Therapy demonstrated its telepsychiatry services to a number of state representatives.
Contact Kristen Thometz: @kristenthometz | (773) 509-5452 | [email protected]
Related stories:
Annual Conference Spotlights Local Efforts to Address Health Inequities
Number of US Overdose Deaths Appears to be Falling
‘I Feel Trapped’: Photos Capture Experiences of People Who Use Drugs
How Chicago Hospitals are Addressing the Opioid Epidemic