Health
What Causes the Flu Vaccine to be Less Effective?
UChicago Study Finds Immune History Influences Effectiveness

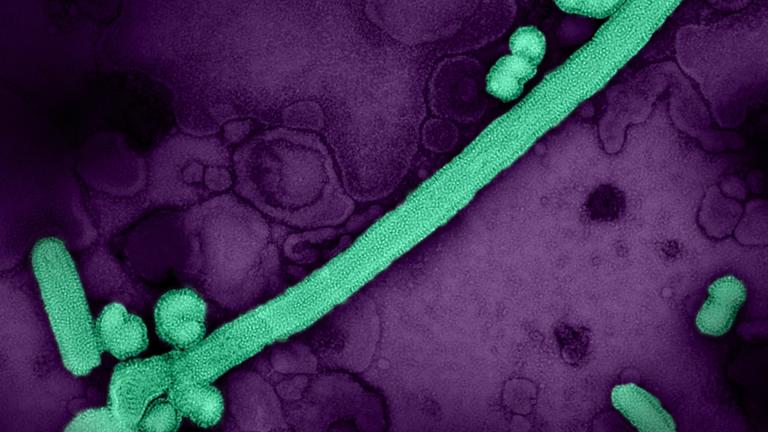
This year’s flu vaccine is only 36 percent effective against influenza A and B, which includes H3N2, the problematic strain currently in circulation, according to the Centers for Disease Control and Prevention.
A flu vaccine’s low effectiveness is often attributed to problems with how it’s designed and produced. Sometimes the flu strains chosen for the vaccine are a poor match for those that end up circulating, especially in years when the H3N2 strain predominates. In addition, most of the flu vaccines administered around the world are grown in eggs, which can cause the virus to mutate and differ from circulating strains, making the vaccine less protective.
But a new study suggests that a person’s past flu experiences could influence how effective the flu vaccine is for them.
During the 2012-13 flu season, the vaccine was only 39-percent effective. Public health officials thought the adaptations in egg-grown vaccines were to blame. But an analysis revealed that poor immune responses – not egg adaptations – may explain the low effectiveness of that year’s vaccine.
“Egg adaptations have variable effects,” said Sarah Cobey, assistant professor of ecology and evolution at UChicago and lead author of the study, in a statement. “Sometimes they matter and sometimes they don’t, but what seems to make the most difference is immune history.”
Flu vaccines are designed to get the immune system to produce antibodies that recognize the specific strains of the virus someone may encounter in a given year. The antibodies target unique sites on the virus and latch onto them to disable it. Once the immune system has antibodies to target a given site on the virus, it reactivates the same immune cells the next time it encounters the virus.
Each year the virus changes ever so slightly, which can be problematic. While the site the antibodies recognize could still be there, it may no longer be the crucial one to neutralize the virus. Antibodies produced from a person’s first encounters with the flu, either from vaccines or infection, tend to take precedence over ones generated by later inoculations. If someone has a history with the flu, the immune response to a new vaccine could be less protective even when the vaccine is a good match for a given year. The vaccine could also induce a weak immune response in many who receive it.
“We see that both vaccinated and unvaccinated people were infected with similar flu viruses and that the vaccine didn’t elicit a strong immune response from most people in our study,” said Yonatan Grad, assistant professor of immunology and infectious diseases at the Harvard T.H. Chan School of Public Health and co-author of the study, in a statement.
Researchers often test how well infection or vaccination to different flu strains protects people from infection with another strain in lab animals, like ferrets. During the 2012-2013 flu season, ferrets immunized with the egg-adapted strain had a poor antibody response to the H3N2 strain circulating that year, causing officials to believe egg adaptations were to blame.
But when researchers in the latest study analyzed blood samples from people who were vaccinated that year, they found no difference in antibody responses to the vaccine or the circulating strains. According to researchers, it seemed their immune systems didn’t bother to recognize the differences from the egg mutations because they already recognized many other sites on the vaccine strain.
“Imagine influenza viruses are like different makes and models of cars,” said Grad. “The ferrets, which hadn’t seen influenza before, learned to tell the difference between closely related strains – like telling the difference between a Honda Civic and a Toyota Camry. But people didn’t distinguish between them and instead just saw cars.”
That doesn’t mean egg adaptations are irrelevant. In a separate 2017 study, Cobey, along with a team of University of Pennsylvania researchers, found that egg adaptations did cause mismatches in the most common vaccine given during last year’s flu season which was dominated by the H3N2 virus.
Newer vaccines can also be grown without eggs, either in insect cells or dog kidney cells, and are much less likely to develop mutations that cause them to be less effective against the flu. But these vaccines have been much more expensive. Researchers hope continuing research will help shift the focus to these more effective vaccines.
Contact Kristen Thometz: @kristenthometz | [email protected] | (773) 509-5452
Related stories:
 Risk of Getting the Flu Remains High in Chicago
Risk of Getting the Flu Remains High in Chicago
Jan. 30: City health officials remind residents it’s not too late to get the flu vaccine. “This is a serious year,” said Chicago Department of Public Health Commissioner Dr. Julie Morita.
 Area Hospitals Race to Keep Up With a Demanding Flu Season
Area Hospitals Race to Keep Up With a Demanding Flu Season
Jan. 8: Health officials say the flu is peaking early this year, with 100 more flu outbreaks statewide than at this time last season. How hospitals are handling the increased volume of patients.
 Flu Cases Spike: How to Protect Against This Year’s H3N2 Flu
Flu Cases Spike: How to Protect Against This Year’s H3N2 Flu
Jan. 3: Doctors say the most dominant strain of the flu this season is one that can take a more severe toll on patients who catch it. How to protect yourself from what could be an especially bad flu season in Chicago.