Health
Are Americans Dying Younger? A Closer Look at Report on Life Expectancy
For the first time since 1993, the Centers for Disease Control and Prevention and the National Center for Health Statistics report that the average U.S. life expectancy has decreased. The numbers appear to indicate that on average, life expectancy for the U.S. population decreased from 78.9 years in 2014 to 78.8 years in 2015. Is it time to sound the alarm for public health, or is this just a blip on the radar?
Joining us to discuss the report are Dr. Diane Lauderdale, professor and department chair of epidemiology at the University of Chicago; and Dr. Richard Cooper, professor and department chair of public health sciences at Loyola University Chicago.
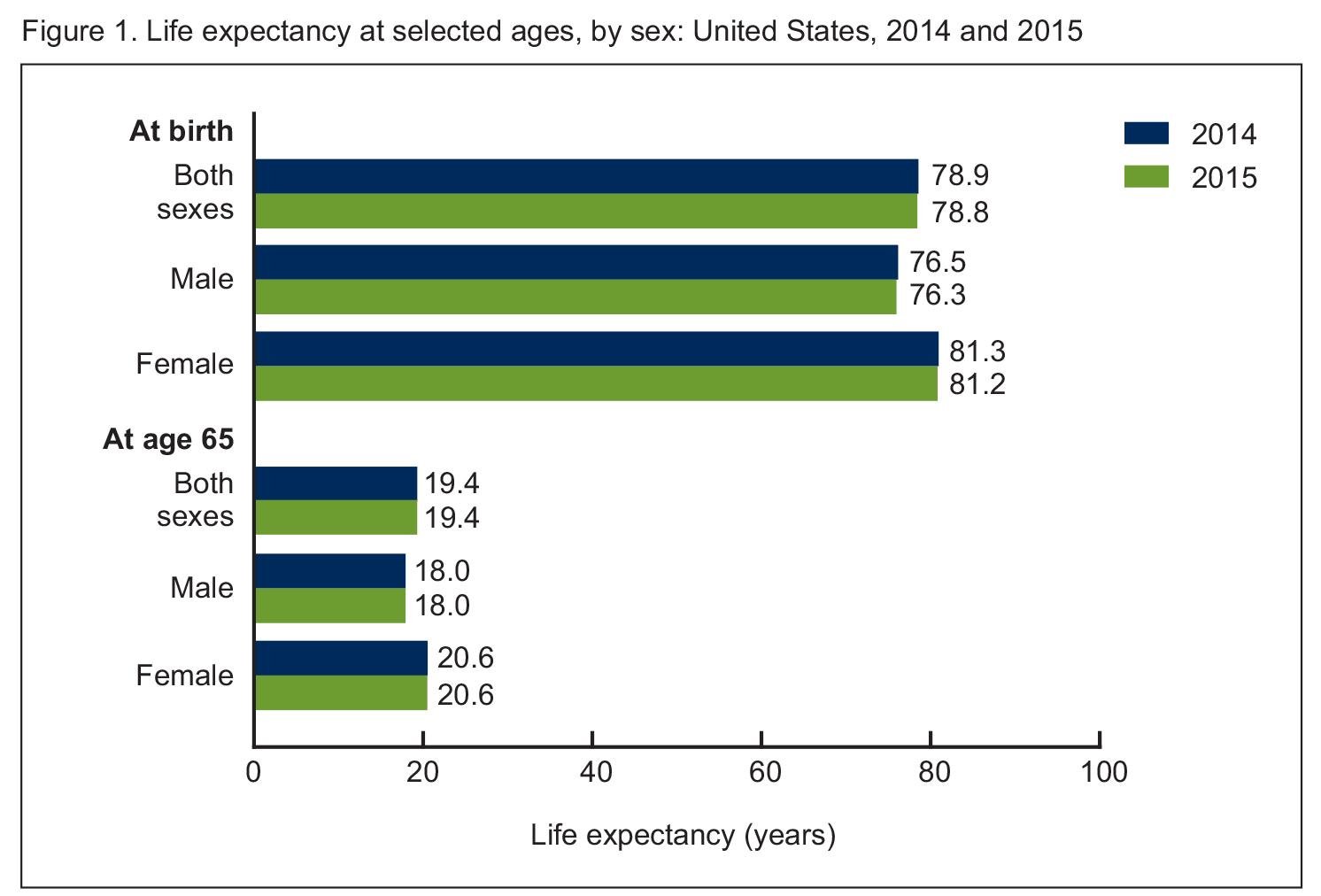 (Courtesy National Center for Health Statistics’ report “Mortality in the United States, 2015.”)
(Courtesy National Center for Health Statistics’ report “Mortality in the United States, 2015.”)
Below, a Q&A with Lauderdale and Cooper.
![]()
This report is preliminary and limited in its scope. Is this one-year drop a blip on the radar or a canary in a coal mine, indicative of a larger trend?
Dr. Diane Lauderdale: You just can’t tell which it is at this point. There are some odd things about the report – the equivalent report issued a year ago for 2014 actually had different numbers for 2014 than this one, and the ones they had a year ago were exactly the same as the 2015 ones are now. What’s changed is that they revised up life expectancy from their initial report a year ago. So that’s why I think this may be a tempest in teapot.
Explaining what life expectancy is is a little complicated – it’s a statistical summary of all the death rates based at different ages in 2015. It’s not like a forecast of what’s going to happen to people over the next 80 years. It summarizes all the risks of death faced by all these people at different ages.
That report showed that the life expectancy at age 65-plus is the same this year. So whatever changed, changed for people who are younger than 65. However they have the age-adjusted death rates from different causes, and the biggest increase is for Alzheimer’s, which is a big increase, except all of those are over age 65. Nobody dies from Alzheimer’s before 65. So one really needs to see the cause of death distribution within age groups – which they don’t usually publish for a few months.
 It’s complicated – this is 2.7 million record data file. It takes them a while together to get together and clean up.
It’s complicated – this is 2.7 million record data file. It takes them a while together to get together and clean up.
I’ve been reading up on different people’s comments on it, and there are a couple of people who went on and on about how this must be the obesity epidemic. And there’s no reason to think that because the two causes of death that appear to increase the most are Alzheimer’s and accidental deaths, which don’t seem relevant to obesity.
The one that is probably really something meaningful is the accidental deaths because there, separate data indicated that heroin and synthetic opioid deaths have really gone up a lot.
The cause of death is not perfect data on a death certificate. Sometimes you don’t know whether it’s accidental or suicide just like sometimes you don’t know whether the underlying cause is heart disease or diabetes or kidney disease since they all co-occur. It’s not always the cleanest data even when people are trying hard, the physicians filling them out, they don’t always know what’s going on.
If there is a slight increase it is white men and women and black men, and not black women or Hispanic men and women. That’s what the report is showing – that’s interesting as well – it’s also not very consistent with obesity as the cause. Apparently the first thing one should be thinking about is fentanyl – synthetic opioids.
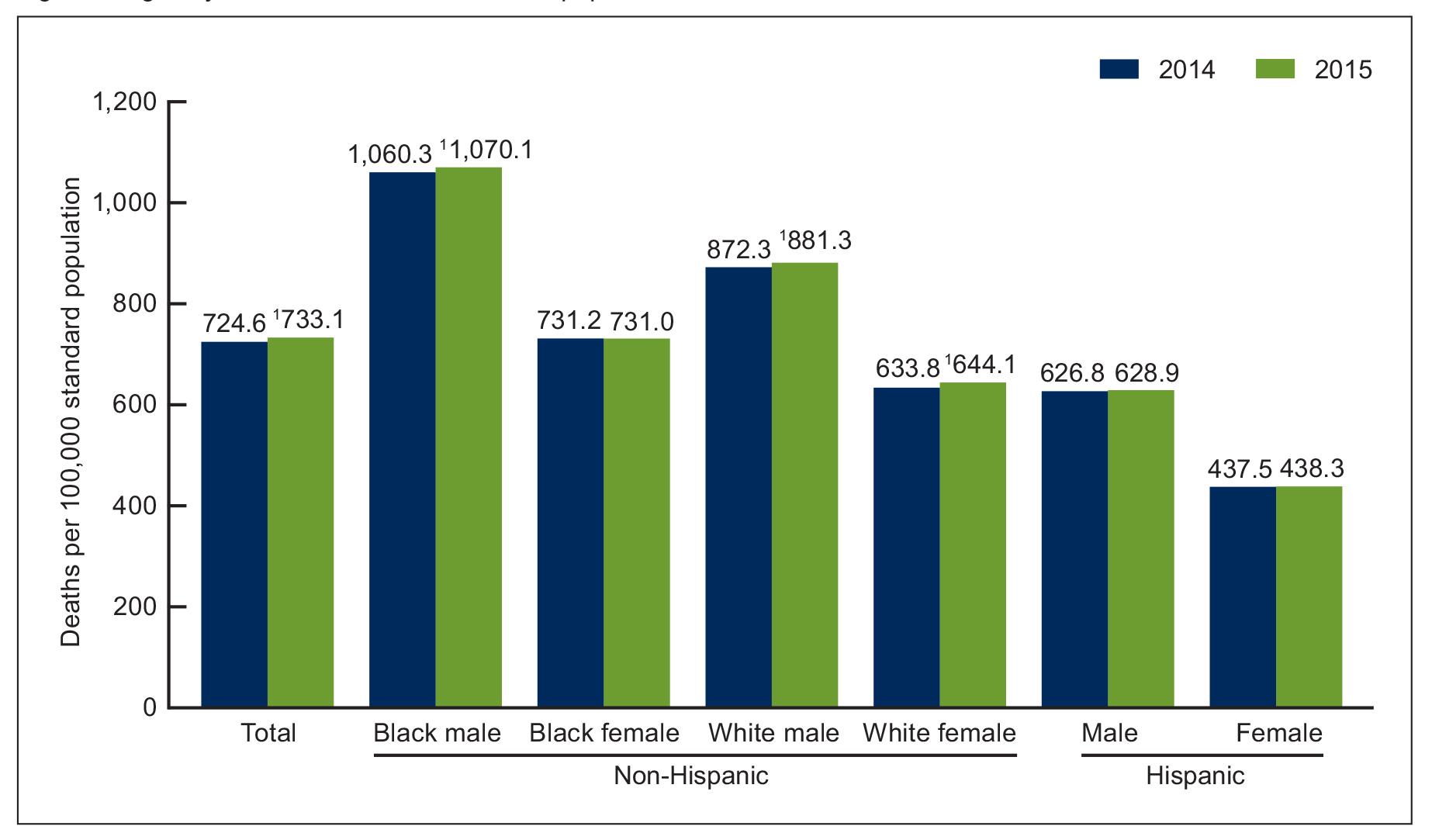 (Courtesy National Center for Health Statistics’ report “Mortality in the United States, 2015.”)
(Courtesy National Center for Health Statistics’ report “Mortality in the United States, 2015.”)
Do you think it’s good for preliminary reports like this to get media attention?
Dr. Richard Cooper: There are two parts to the issue – what’s going on long term and what’s going on this last year. The decrease in life expectancy is superimposed on a slowing of the overall process of mortality reduction. Before 2010 life expectancy was getting longer fairly rapidly; since then it’s stagnated. For men, it was ... opiates, poisonings, accidents – for women it was primarily Alzheimer’s going up (this last year).
The analogy I was thinking about is a bank account: You have credits and debits, but it’s also important to know what you’re spending it on and that – I think it’s probably appropriate to talk about the middle-aged men – it’s an important thing. It probably should be highlighted in some way.
Compare the U.S. health system to other developed countries’ health systems – is there a life expectancy correlation? What are contributing factors to the divergence?
Lauderdale: We have strikingly low life expectancy compared to equally wealthy nations. We do have big race disparities – other countries do not have that. Something that makes our health look better than it would otherwise is that we have a substantial number of immigrants who generally have lower mortality rates; have better life expectancy than the U.S. born. And that’s probably because it’s actually hard to immigrate – it’s like a test that somebody has passed which shows they’re able to figure out all kinds of things. And also people at the point when they immigrate, they probably had good health and good mental health. All those are predictors of greater longevity.
Health habits, diet, physical activity, as well as the health care system, it’s generally a stressful country with high income inequality.
Cooper: Long term – the major factor is that we have a lot more people in severe poverty than anywhere else – about a third of children grew up in poverty. That’s what’s been keeping us behind. Other countries are seeing an increase in life expectancy and much lower rates of the miscellaneous causes – homicide, accidents, poisoning, suicide.
For stroke, we’re among the lowest in the world. The problems that characterize our society – violence, isolation, high rates of poverty – those are the difference.
Other historical dips are correlated with major health crises, like AIDS or flu outbreaks. How did the government respond to those, if they did at all? How, in your opinion, should the government respond to this report?
Lauderdale: The heroin and opioids need a public response. It’s not clear what else in here is actually happening in ways that we’re not already doing our best to try to address. If there is something that is specific to this period of time that’s driving the stagnation or even declining life expectancy, it probably is the drug problem and that’s something the government can address.
Over the last decades, the U.S. has looked worse than other wealthy nations and those are broader issues that are harder to address. It’s not any one thing. Some of it is health habits, some is health care, some are social factors that are beyond the public health and medical establishment to address.
It’s this complicated stream of all the death certificates filled out all over the country that makes their way to the state offices that then go to the National Center for Health Statistics, and then you need a denominator for those fractions, and those are coming from the Bureau of Labor Statistics and the decennial census and then their ongoing data collection to estimate the population. So it’s putting together all those data collections to figure out the death rate.
And then the cause of death data is a little complicated too. You rely on every single doctor and coroner to do their level best to really think hard and figure out what the underlying cause is, not the immediate cause. It may well be that this – for over several years now – that Alzheimer’s as a cause of death has increased, but that may simply reflect the fact that there’s a decrease in stigma rather than putting in something more general, (like) cardiovascular diseases.
Over the last two years there has been a decrease in the age-adjusted deaths attributed to cancer – and that probably is real and reflects real improvement in therapy.
Cooper: I think the only one that was big enough to deserve a comparison was the emergence of AIDS, and I think the story is that there was a very vigorous and effective campaign to get something done about it and so the development and distribution of drugs was speeded up and also prevention (efforts). That was a direct reflection of government intervention.
The only other kinds of epidemics are really flu, and they try to come up with a good vaccine. There’s a phenomenon called harvesting the susceptibles – when someone is quite ill but hanging on, but there’s something like the flu, they die sooner than they would’ve and the next year they have an extra drop in the statistics. But we haven’t had major flu outbreaks since 1968.
But we are beginning to pay a big price with diabetes – that’s the one that people should be screaming about that deserves attention. We haven’t appreciated the significance of it – at the age of 40, half the population is either diabetic or pre-diabetic.
The way people use public health indicators – like I said, it’s like your bank account. The variety of things you spend your money on, the summary doesn’t tell you that – you need several statistics if you want a well-rounded picture. In the U.S. we do have very rich data sources – we can describe our failures with great accuracy.
Related stories:
 Experimental Alzheimer’s Drug Fails in Large Study, But Hope Persists
Experimental Alzheimer’s Drug Fails in Large Study, But Hope Persists
Dec. 9: Disappointing results from a clinical trial released late last month by Eli Lilly, but the drug is still being studied as a potential therapy for those who are at risk for memory loss.
 Study: Treating Malnutrition Shortens Hospital Stays, Decreases Readmissions
Study: Treating Malnutrition Shortens Hospital Stays, Decreases Readmissions
Dec. 8: Addressing hospital patients’ malnutrition can reduce patient stays by nearly two days and decrease hospital readmissions by nearly 30 percent, according to a new study.
 The Future of HIV/AIDS: Treatment, Prevention 35 Years Later
The Future of HIV/AIDS: Treatment, Prevention 35 Years Later
Nov. 29: A look at some breakthrough treatments for HIV and AIDS and a landmark clinical trial for a vaccine ahead of World AIDS Day.






