Ahead of World AIDS Day on Thursday, we take a closer look at the AIDS epidemic 35 years later.
It was June of 1981 when the Centers for Disease Control and Prevention published its first report about the mysterious death of five young, previously healthy gay men. Treatment of HIV has drastically changed over the last three and a half decades.
The current prognosis: people living with HIV have the same life expectancy of people without the disease, if properly diagnosed and medicated.
However, the infection rates of gay and bisexual men of color are rising. The CDC predicts that half of all African-American men who have sex with men (MSM) will be infected with HIV in their lifetime. The study also estimates a quarter of all Hispanic MSM will be diagnosed with HIV within their lives if current HIV diagnosis rates persist.
There’s still no cure but there are several major breakthroughs in HIV treatment and research.
We spoke about the latest treatments, vaccine clinical trial and possible cure with Dr. Magda Houlberg, the chief clinical officer at Howard Brown Health, a federally qualified health center that primarily serves the LGBTQ community at six sites, from Englewood to Rogers Park; and Dr. Abbas Hyderi, associate dean and associate professor of clinical family medicine at the University of Illinois at Chicago College of Medicine. Hyderi focuses his practice on HIV and lesbian, gay, bisexual and transgender health. Hyderi is also a board member of the AIDS Foundation of Chicago.
Below, an edited Q&A with Houlberg and Hyderi.
There have been many strides in HIV treatment but no cure. Let’s start with the PREP pill. In a 2015 study of 600 sexually active people in San Francisco, no one was infected with HIV while on PREP. So what is PREP and how has it revolutionized treatment of HIV?
Dr. Magda Houlberg: Prep is a medication to help prevent HIV infection. It’s one pill taken once a day. It’s a very effective tool. Patients have more control over own health.
Dr. Abbas Hyderi: PREP is one tablet with two medications. It has revolutionized the prevention of HIV because it’s nearly 100 percent effective. Condoms are only 90 percent effective with breakage and misuse. When taken daily it’s effective–so consistency is critical.
The CDC reports one in three health care providers are not aware of PREP. So providers and patients don’t know about PREP. How do you change that?
Hyderi: Sometimes physicians fall under specialization so they think HIV isn’t in their wheelhouse. There’s an opportunity for providers to be educated and to raise awareness. Patients come in for all kinds of reasons including physicals, so universal HIV testing is important. It’s incumbent upon providers to ask questions about social and sexual history to determine if your patient is of higher risk of HIV infection. We don’t do a good job asking about social and sexual history. Doctors need to know so they can order a standard set of labs and to prescribe HIV prevention. It involves awareness and training.
There’s a treatment if you’ve been exposed to the HIV virus called PEP. What is it and how quickly does a person need to get treated for it to work?
Houlberg: PEP is short of Post-Exposure Prophylaxis. It’s effective within 72 hours after exposure. It’s actually three medications taken for 30 days. In health care exposures (providers stuck by needles, etc.) it’s up to 99 percent effective. The tricky part is to get people in for treatment within the window. A lot of medical providers don’t know about PEP so getting the word out is critical. Cost doesn’t have to be a barrier because it's covered. More education is needed. If people know about it, then patients will drive demand.
These drugs require adherence to the regimen. But is that realistic for some of your patients and is there a better way with long-acting injections or implants?
Houlberg: There will be a longer-acting PREP down the road. Implant or injections are being investigated. Sticking to a medication regimen can be challenging for some patients. But for our patients at Howard Brown Health, they’re highly motivated so they comply with PREP.
Hyderi: Patients vary. Most of my patients have been fine with taking their meds regularly. My patients span the socioeconomic area, but if there are difficulties to access to healthcare, then it can be a problem because these medications require ongoing bloodwork and lab monitoring.
According to a CDC projection, half of all black men who have sex with men (MSM) and 25 percent of Hispanic MSM will be infected by HIV in their lifetime. Why do you think the rate of infection is increasing?
Houlberg: Access to HIV treatment is an issue. People also may not be aware of their HIV infection. Access to PREP is an issue. People don’t know it’s an option and that it’s safe to use. It also has to do with sexual networks: if there’s HIV within your sexual network, there’s more of a chance meeting someone who is infected. There’s also access to basic care and prevention.
Hyderi: There are a lot of risk factors for exposure to HIV and transmission to others. A lack of access to healthcare, a lack of ability to get meds and to follow up on meds are all big barriers. African-American communities are dealing with poverty, lack of access to housing and healthcare and a lack of access to clean needles and syringes. There definitely are social factors at play.
A team of researchers at Temple University are searching for a cure and have pioneered a ‘gene editing’ technique by cutting out the virus from human cells. Researchers from the National Institutes of Health found an antibody that neutralizes 98 percent of HIV strains. There’s no cure yet, but promising things on the horizon?
Hyderi: The HIV virus mutates really rapidly and then also replicates very quickly. It’s difficult to come up with a vaccine to neutralize and cover all the different strains of HIV. It’s very promising they found an antibody that stops HIV in its tracks or can trigger the immune system. With the gene breakthrough at Temple University, they can render HIV permanently inactive by accessing the viral DNA. That means it would lack the ability to infect the other cells. We hope it’ll move to human clinical trials by 2019.
The NIH trial with N6 has neutralized 98 percent of HIV antigens. A vaccine needs to have both strong potency and strong breadth to cover the various strains of HIV. A study in England brought out sleeping/dormant HIV cells. Combining it with N6 could permanently get rid of HIV. That combination means we’re closer to a cure. They’ve studied N6 in monkeys and now in small human trials in phase two trial but no crystal ball of when there will be a cure. Time will tell. Only one patient has been cured so far and that’s because had bone marrow transplant to cure him of cancer.
Why has it been so tough to pin down a cure?
Houlberg: There are a number of factors. HIV can hide out in different cells and tissues in body. We call that a reservoir of HIV. The gene therapy is promising. There’s that and other ways that are moving toward cure potentially within our lifetime. Both are a ways away from being studied in humans. But those types of things may yield a cure.
So the outlook for people with HIV is pretty positive now. It’s treated more like a chronic illness rather than a death sentence like it was back in the ’80s?
Hyderi: Absolutely. To give you a sense of things, when I was a medical student in the 1990s, it really was a death sentence. Then protease inhibitors came along and those were a game changer. Back then you took 20 pills a day, both with and without food, which had lots of side effects and was difficult to tolerate. Now, it’s one pill once a day. That’s phenomenal. It makes it much easier to remember to take, the medicine in that one pill is stronger and there are fewer side effects. If patients take their meds consistency, their life expectancy is same of those without HIV.
Houlberg: When people living with HIV have access to care, transmission goes to zero. Prevention work is about getting people into care. Here’s the total package: if your know your HIV status, you’ll know that those treatments are available. Access to treatment with PREP will reduce HIV transmission. The communities most impacted by HIV have issues with access to health care and that is usually a socioeconomic issue. We have the technology to create an AIDS-free generation but to change the tide, it’s a matter of getting to people who really need the treatments and preventatives.
Editor's note: This story was updated Nov. 30 to correct the daily dosage of prep mentioned by Dr. Magda Houlberg: “Prep is a medication to help prevent HIV infection. It’s one pill taken once a day,” she said.
More health news:
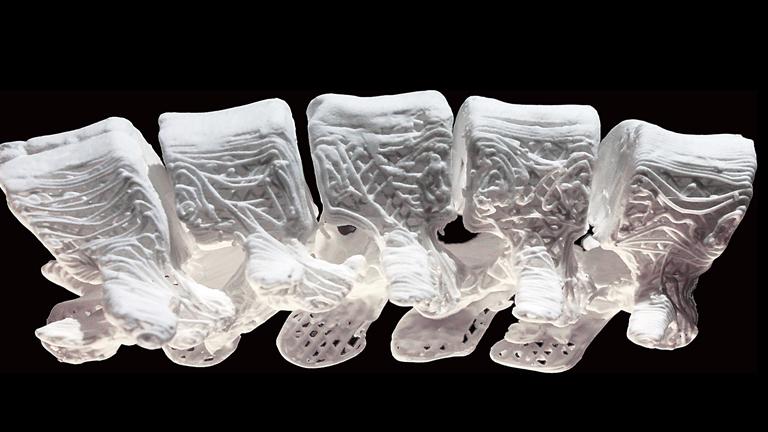 Northwestern Scientists Create Synthetic Bone Using 3-D Printer
Northwestern Scientists Create Synthetic Bone Using 3-D Printer
Sept. 28: New technology developed in Chicago could lead to major advances in healing broken bones and other sports medicine injuries.
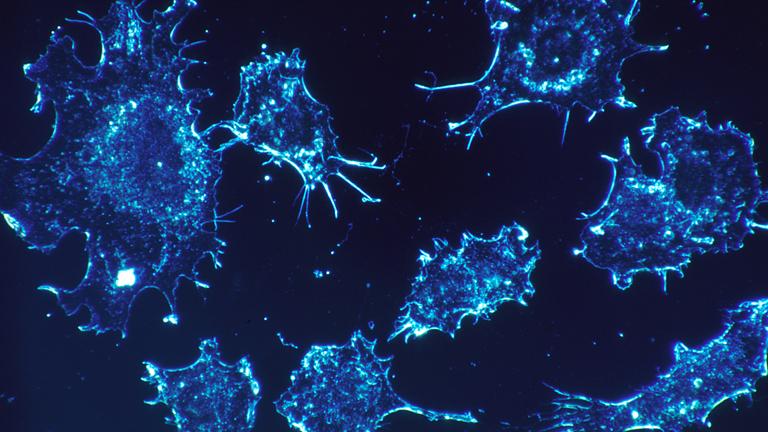 U of C Researchers Develop Therapy to Treat Lethal Cancers
U of C Researchers Develop Therapy to Treat Lethal Cancers
Sept. 21: A new form of cancer treatment developed by University of Chicago scientists was so effective in studies that one researcher said it’d be a “breakthrough” if it were replicated in humans.
 Head of Mayo Clinic Addresses ‘Epidemic of Burnout’ Among Physicians
Head of Mayo Clinic Addresses ‘Epidemic of Burnout’ Among Physicians
Sept. 14: The head of the Mayo Clinic sheds light on what he has called “an epidemic of burnout” impacting doctors and undermining patient care.