Patti Beyer (Jon Hillebrand / NorthShore University HealthSystem)
Patti Beyer (Jon Hillebrand / NorthShore University HealthSystem)
For years, Glenview resident Patti Beyer got an annual a mammogram and each year her results were normal. Yet in 2016, she was diagnosed with invasive breast cancer.
“I was told the cancer had been there for quite some time,” said Beyer, who admitted that her most recent mammogram prior to the diagnosis had been 17 months earlier due to her husband Bud’s cancer diagnosis. (He is alive and well, by the way.)
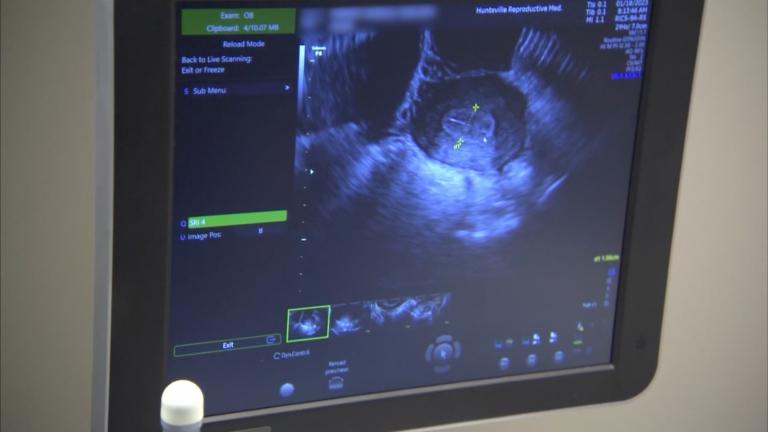
But Beyer’s cancer wasn’t found on a mammogram. Instead, it was detected by an automated breast ultrasound, a test Beyer requested at the behest of her sister, who lives in California, where state law requires that women who have dense breast tissue are notified if it is detected and alerted that it might increase their risk of breast cancer. Illinois does not have such a law, but Beyer knew she, like her sister, has dense breast tissue because a radiologist mentioned it to her in 2007.
That ultrasound she requested spotted a lesion. “They called me the next day and I had three mammograms, which were all normal,” Beyer said. A needle biopsy revealed she had breast cancer.
Fortunately, Beyer’s cancer was small (measuring less than 1 centimeter in size) and detected early. “I was very sad about getting breast cancer, but it’s hard for me to complain at all because I was able to choose a lumpectomy and my cancer survival [rate] is very good because it was caught at an early stage,” she said.
Beyer doesn’t have a family history of breast cancer, but dense breast tissue is a risk factor for the disease – and, in fact, was her only risk factor. According to the American Cancer Society, women who have dense breast tissue have a “slightly” higher risk of developing breast cancer than those who do not.
Beyer is now on a crusade to get a breast density notification law passed in Illinois. “A woman, I feel, has a right to know,” she said. “It’s already in the mammography report to the doctor but unless the doctor tells you it’s kept from you.”
Across the country, 31 states have mandatory breast density notification laws, according to Are You Dense, Inc. (AYD), an advocacy group founded by Nancy Cappello, Ph.D. after she was diagnosed with stage 3 breast cancer despite 11 years of normal mammogram results. Cappello is pushing for a federal law and works with groups across the country to pass breast density notification laws.
“I never missed a mammogram,” said Cappello, who was diagnosed with breast cancer six weeks after receiving a normal report. An ultrasound revealed she had invasive cancer that had spread to 13 lymph nodes. “I asked my doctors why I was diagnosed so late. And my doctors said in a nonchalant manner, ‘Nancy, you have dense breast tissue. It’s hard to see cancer in dense tissue.’”
How Dense Breast Tissue Masks Cancer
Breast density is classified by radiologists into four categories, ranging from all fatty tissue to extremely dense with very little fat, according to the American Cancer Society. (Courtesy of Are You Dense, Inc.)
Breast density is only seen on mammograms and isn’t detected based on how a woman’s breasts feel, according to the ACS. Radiologists classify breast density into four categories that range from almost all fatty tissue to extremely dense with very little fat and higher percentages of fibroglandular tissue. Up to 40 percent of women worldwide have dense breast tissue, according to AYD.
“Fibroglandular tissue appears white on a mammogram and breast cancer appears white on a mammogram so it can mask or hide cancer in women with dense breast tissue,” said Dr. Georgia Spear, who heads NorthShore University HealthSystem’s department of breast imaging and read Beyer’s radiology reports when she was diagnosed with cancer. “It can hide cancers and can miss up to one-third of breast cancers in women with dense breast tissue with a mammogram screening, which is the gold standard [of screening] at this time.”
Mammograms do detect the most common types of breast cancer, which form in the milk ducts of the breast, by detecting the calcification caused by abnormal cells within the milk ducts. Calcification appears white on mammograms and can only be detected by mammograms – even in women with dense breast tissue.. “They’re the gold standard for reasons in that they detect calcification in early breast cancer and that can’t be found under an ultrasound or other modalities,” Spear said.
When cancer spreads outside of the breasts’ milk ducts, it becomes invasive and may not be detected by mammograms in women with dense breast tissue. “Using an ultrasound we can overcome the superimposition of tissue and can detect the small invasive cancers that we couldn’t otherwise see in women,” said Spear, who views mammograms and ultrasounds as complementary tools.
‘Why wait to be the last one?’
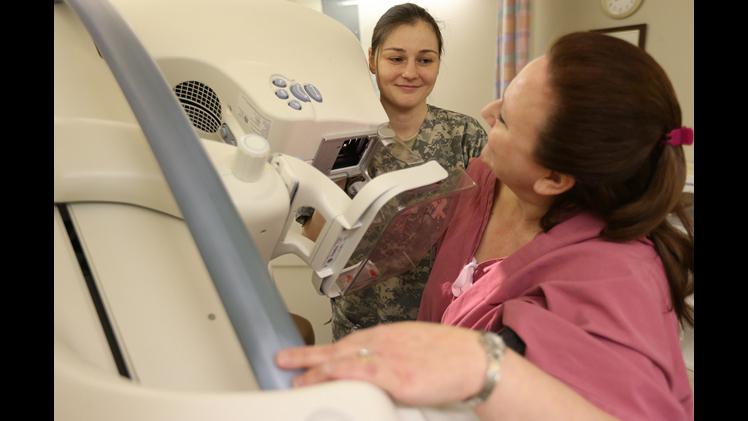 (Army Medicine / Flickr)
(Army Medicine / Flickr)
Despite the lack of a statewide law, some Illinois facilities are already notifying patients, including the University of Chicago Medicine and NorthShore University HealthSystem.
Patients of NorthShore can access their mammography reports through the system’s patient portal, according to Spear. Patients are informed of their breast tissue type and that “supplemental screening with ultrasound should be considered with ultrasound due to their tissue type,” she said.
Spear said she’d be supportive of legislation that would require notification if a mammogram reveals dense breast tissue. “With improved legislation, we can increase patient education and increase access to supplemental screening for women with ultrasounds who need them,” she said.
Beyer, who is spearheading the initiative in Illinois, said she’s spoken with state Sen. John Mulroe and Rep. Michael McAuliffe, who tried to get a bill passed in 2014, when only about a dozen or so states had mandatory breast density notification laws. Now that more than 30 states have such laws, Mulroe thinks legislation might have a better chance at passing. They plan to introduce a new bill next session.
“If medical professionals are already doing it in 30 other states and they’re OK with it, I think it’s a better argument that we should be doing it here,” Mulroe said. “Why wait to be the last one?”
The Illinois State Medical Society said it would evaluate any new legislation as it’s introduced and declined to comment on previous efforts to get such a law passed.
But in 2014, the ISMS voiced its opposition to legislation that would have mandated mammography reports sent to patients include information stating dense breast tissue makes it more difficult to identify cancer and may be associated with an increased risk of cancer.
“ISMS opposed this language because this bill would legislate the practice of medicine. There is also no consensus within the scientific community on the relationship between breast density and cancer risk,” ISMS wrote in a 2014 report to its members. “Furthermore, there is no reliable method for assessing breast density, and no clinical guidelines that recommend additional screening solely on the basis of high breast density.”
Guidelines from the ACS or American College of Radiology do not address supplemental mammography screenings with ultrasound as of yet, Spear said. She’s leading a three-year study using automated breast ultrasound as a supplemental screening for breast cancer. A previous study revealed a cancer detection rate of 12 per 1,000 using supplemental ultrasound screening.
“This is why research that we are performing right now on automated breast ultrasound is so important. One of the goals of our prospective research study is to help establish much needed practice guidelines,” Spear said.
The ISMS offered an amendment that removed the mandate and replaced it with changes to the written summary on breast cancer already published by the Illinois Department of Health to include information on the meaning and consequences of dense breast tissue. The amendment was adopted and signed into law.
Despite the lack of a dense breast notification law, Illinois is ahead of the curve in terms of requiring insurance companies to provide coverage of breast tomosynthesis (or 3-D mammography), as well as provide an ultrasound (SB1365) or MRI (SB0314) if a woman is found to have dense breast tissue.
“Illinois has one of the best insurance coverage laws in the nation for dense breast tissue,” said Cappello. “It’s interesting because while Illinois has a great ultrasound coverage law and also come January they’ll have an MRI coverage law – which is just phenomenal – what typically happens is women in the state don’t even know they may need these tools because they don’t even know they have dense tissue. ... So still unless a doctor is discussing dense breast tissue with his or her patient, most women wouldn’t know they had it unless it’s being reported to them.”
Beyer said the lack of a state notification standard is creating inequity, with some women finding out they have dense breast tissue while others don’t. She says she’s been to many events where women have told stories about having years of normal mammograms only to be diagnosed with late-stage breast cancer. None of them were informed they had dense breast tissue prior to their diagnosis, Beyer said. “That’s the horrible thing.”
Knowledge of her own dense breast tissue allowed her to seek out supplementary screening tools which detected her cancer early. “That’s what notification can do,” she said. “It can give you an early diagnosis.”
Beyer has created a Facebook page to raise awareness and support for her effort to get a dense breast notification law passed in Illinois.
Note: An earlier version of this story incorrectly described how Beyer learned she had dense breast tissue and breast cancer. The story has been updated. We have also clarified the ISMS’s opposition to past legislative efforts.
Contact Kristen Thometz: @kristenthometz | [email protected] | (773) 509-5452
Related stories:
 ‘Left Boob Gone Rogue’ an Insightful, Humorous Blog About Breast Cancer
‘Left Boob Gone Rogue’ an Insightful, Humorous Blog About Breast Cancer
Aug. 29: Meet the Chicago physician who writes about her personal experiences dealing with breast cancer.
 Report: Despite Progress, Illinois Can Improve Cancer-Fighting Policies
Report: Despite Progress, Illinois Can Improve Cancer-Fighting Policies
Aug. 3: While Illinois was lauded in a new report for its smoke-free laws and rules on indoor tanning devices, the state is “exceptionally” far behind on comprehensive tobacco-control programs, according to a national cancer advocacy organization.
 Chicago Leads Nation in Reducing Racial Disparity in Breast Cancer Deaths
Chicago Leads Nation in Reducing Racial Disparity in Breast Cancer Deaths
Aug. 2: For black women in Chicago, a breast cancer diagnosis in 2003 meant you were 68 percent more likely to die from the disease than a white woman. A new study shows that gap is closing.