Health
What Role Should Data Analysis Play in Health Care Policy?
In 2008, health care policy researchers got a lucky break: The state of Oregon announced that it was drawing names by lottery to enroll low-income adults in its Medicaid program, creating an unprecedented opportunity for a controlled, randomized study of Medicaid coverage and its effect on, among other things, health care utilization.
Since then, the Oregon health care experiment has been used to buttress arguments for both reducing and expanding Medicaid.
What role should these kinds of studies play in crafting public policy? Can they lead to better health care? And what does better health care mean?
Joining us in discussion is one of the study’s authors, Katherine Baicker, dean of the University of Chicago Harris School of Public Policy.
Below, a Q&A wit Baicker.
![]()
You’re an advocate of what you call evidence-based health care policy. Can you explain what that is?
There are a lot of things that sound like great ideas that don’t pan out in the real world. Bringing evidence to bear on which policies are effective, and at what cost, in making rational effective policy. (We) need to know what the cost is, what benefits they provide. Both need evidence. We can theorize about whether a program might save money but only in the real world can we see how it pans out. But knowing what the cost and benefits are doesn’t tell us what the right policy is. We want elected officials to weigh those costs and benefits and come to a decision consistent with their policy priorities. I don’t pretend that the evidence tells us what the right answer is, but it ought to be grounded in what the evidence supports.
How can government implement EBHP?
The kind of rationale I would like to see play out more broadly – for instance, Medicaid and whether to in the past expand or now contract Medicaid or turning it into block grants, there’s a raging debate on what Medicaid does for enrollees. So, on the one hand we have the idea that expanding Medicaid will save money because ER visits will go down, people will better manage their health conditions, go back to work and pay taxes, and put all that together and insurance saves money. One the other, we have people saying that insurance is really costly and doesn’t help people, Medicaid is a terrible insurance program and people don’t get much access to care, expanding the program doesn’t do anyone any good. Neither of those stories is true. The optimistic view says that it has huge benefits and pays for itself, pessimistic view says it has huge costs and no benefits. Like most programs, it has benefits to people who enroll – people on Medicaid are much better off – but it costs more.
So the question is, are the benefits to enrollees worth the cost and alternative uses for those funds. Would I rather spend public money on Medicaid, infrastructure, education, lowering taxes? Saying Medicaid doesn’t help enrollees, or that it’s free, isn’t evidence-based. There is now a commission on evidence-based policy that has a series of recommendations about promoting the development of evidence, making sure that researchers have data they need and that the evidences gets into the policymakers hands, but we ought to ensure that the evidence is there and incorporated into their decision making.
What can researchers do to mitigate politicization of their research?
(They can be) really careful and disciplined to not make recommendations based on their research. Journalists, policymakers, lots of people ask me and my colleagues, so does your study say we should expand Medicaid or not? And my response is, this study can tell you costs and benefits of doing that, but how you weigh that is up to you. That is a difficult position to be in, because as a voter I have my own views. As a citizen, there are policies I prefer. But it’s important that I keep those “informed citizen Kate” views separate from the “scientific evidence-generating Kate,” because policymakers need to be able to apply their own to give the unvarnished truth about policy without layering on our own values. I don’t think every researcher agrees with me on that stance, but I think it’s the only way to make sure evidence is taken seriously. Different people can and ought to have different views on what the most important policies are. Some people care more about kids’ education, vaccination, roads and infrastructure – all those things are important, but we live in a world of budget restraints, and there are tough tradeoffs in all of these things. They ought to be making them based on a common set of facts.
How do you anticipate work requirements for Medicaid will affect the opioid crisis?
Having medical coverage could affect the opioid crisis in a couple different ways. We’re still gathering evidence. On one hand, having insurance might increase access to doctors and prescriptions, so you might be more likely to get an opioid prescription that has potential to generate addiction. But also, you’d have increased access to treatment for addiction. So one effect suggests increased use, one effect suggests decreased use. I have yet to see evidence that either is the case.
How can we increase value in health care?
There’s ample evidence that we’re not getting as much value out of the health care system as we should – measurable things like longer lifespans, higher quality of life. A lot of that is driven by the way we pay for health care. Too much is paid for based on volume rather than value or quality and I think there’s an opportunity to have innovative insurance coverage so providers are paid more when they deliver high-quality care. That could be bundled payments, shared savings, or global payments, there are a lot of different innovative models for paying providers, but right now I don’t think we’re forming our payments to align with high-quality, high-value care.
There are components of different countries’ systems – there’s a lot to learn from other countries – but there’s not a single system to point to and say, we ought to adopt that. Our population is much more heterogeneous than a lot of small countries with more unified systems, our health needs are different, our system is organized differently, so even if you wanted to adopt one country’s model, it would be difficult to import and have it work the same way. No model is perfect, but thinking about risk adjustment so that insurers don’t have an incentive to enroll healthier people rather than sicker people, competition among insurers offering good insurance packages for people to select among, better information about which processes are more effective, which providers are delivering higher quality services, and paying accordingly.
We know that lots of things affect your health outside the walls of the health care system – where you work, access to healthy environments, food, places to be outdoors, where your kids are going to school. All of those things affect your health. It would be great to think about this holistically – how does transportation affect health, how does education affect health – and marry flexibility with the accounts. Health care resources in general aren’t allowed to be spent on things like, say, air conditioning, but if your goal is to improve people’s health, being able to go out and spend that money on air conditioners and then measure, did it pan out? If it does, great! If it doesn’t, then we have measurable results. So real measurement, real accountability, innovative ways to address problems.
The goal ought to be to take every opportunity to gather data and implement policies in a way that makes it easier to figure out what they’re doing. If you go back to the Oregon study, the reason we got such great information out of Oregon is that the state had a waiting list for its Medicaid program and drew names by lottery because it seemed like the fairest way to allocate. Rarely do we have that opportunity in public policy – I would not advocate for Medicaid to be allocated that way – but there are all sorts of opportunities to measure that we’re not capitalizing on. If we’re going to pilot a program to reduce infant mortality out of five health care centeres, instead of taking the first five that raise their hands, pick 10, and then randomly pick five. It does not cost any more money, but a minor tweak to how you pilot something or phase a rollout can dramatically affect how much you learn. What I would love to have enter the public discourse is having an eye towards can how we can figure out what this program is doing and can we do it in a way that we can learn as much as possible without spending more money or effecting enrollees.
Health care is a hot segment for jobs. Does this work against increasing value in health care?
It’s tempting to think that the more jobs in health care the better because we want high employment rates and more jobs is a good thing, but thinking of our health care sector as an employment program is inconsistent with trying to deliver high-value, quality care we can all afford. Imagine if we could improve care with half the resources. That would be a great thing, because then we can use that money for other things. So we should be thinking about how much health we get out of the health care system as a driving factor. We would never think of saying, let’s employ twice as many people to make cars, because that would just drive up the price of cars and make them less affordable for everyone. If we were to employ fewer people in hospitals because we don’t need hospitals as much – we could retrain them to do other things. It might also be that we should employ people differently – maybe there are too many specialists and not enough nurse practitioners. Those outcomes should be based on where people can improve health most.
Related stories:
 Safety Tips for Exercising Outdoors in Winter
Safety Tips for Exercising Outdoors in Winter
Jan. 12: Don’t let frigid weather derail your outdoor exercise routine. With the proper precautions and gear, you can keep it up all winter long, says orthopedic surgeon Dr. Diego Villacis.
 Area Hospitals Race to Keep Up With a Demanding Flu Season
Area Hospitals Race to Keep Up With a Demanding Flu Season
Jan. 10: Health officials say the flu is peaking early this year, with 100 more flu outbreaks statewide than at this time last season. How hospitals are handling the increased volume of patients.
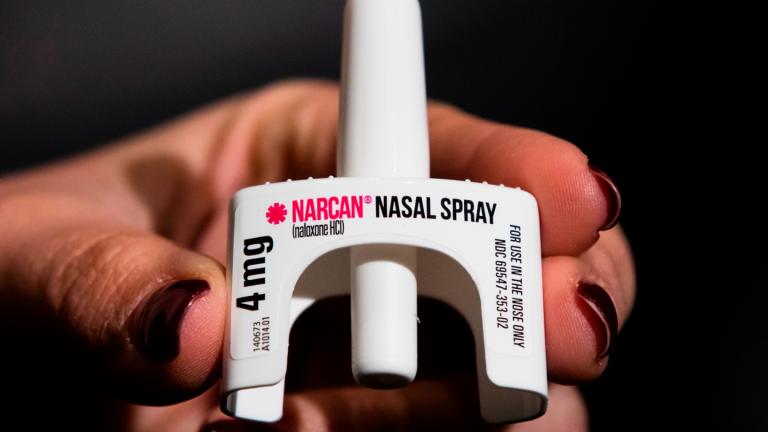
 Illinois Health Officials: State Facing ‘Unprecedented’ Opioid Epidemic
Illinois Health Officials: State Facing ‘Unprecedented’ Opioid Epidemic
Jan. 4: Opioid overdoses in Illinois claim more lives than homicides and car accidents. State health officials tell us what’s behind the crisis.