Health
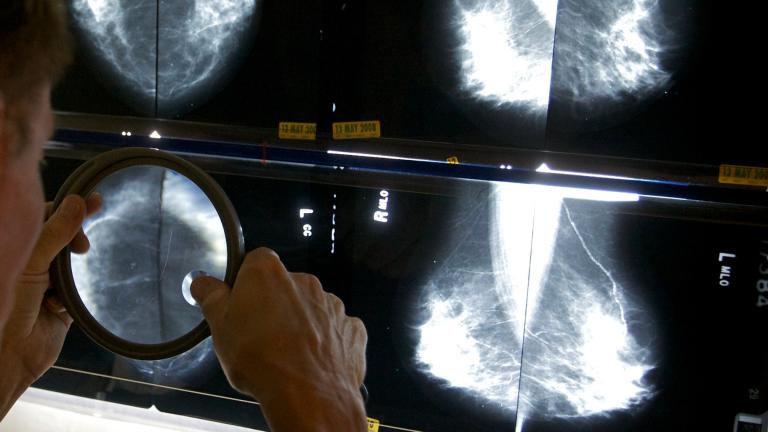
New Guidelines for Breast Cancer Screening
The American Cancer Society has issued new guidelines for women at "average risk" of developing breast cancer, raising the age it says they should start regular mammogram screening from 40 to 45.
Dr. Carolyn Bruzdzinski, vice president of the American Cancer Society's Lakeshore Division in Chicago, and Dr. Kent Hoskins, who directs the Familial Breast Cancer Program at the University of Illinois at Chicago, join us to discuss the changes and to explain how women should go about determining their levels of risk.
Last week, the American Cancer Society released new guidelines for breast cancer screening, which were published in the Oct. 20, 2015 Journal of the American Medical Association.
The new recommendations for women at average risk of breast cancer include:
- Begin regular screening mammography at age 45
- Women ages 45-55 should be screened annually
- Women ages 40-44 should have the option to be screened annually
- At age 55, women should have mammograms biennially (women who want to continue with annual mammograms should be able to do so)
- Breast exams are no longer recommended
Women who are at high risk of breast cancer (due to a family history of breast cancer, a breast condition, etc.) should speak with their medical providers about screening.
Watch the ACS’ video about the guidelines below.
This past spring the U.S. Preventive Services Task Force issued its 2015 draft recommendations for breast cancer screening, which include:
- Biennial mammography screening for women ages 50-74 who are at average risk of breast cancer
- Women who place a higher value on the potential benefit than harms of screening, may choose biennial screening between ages 40-49
The guidelines note that while mammography in women ages 40-49 may reduce breast cancer deaths, it may also result in more false-positive tests and unnecessary biopsies. Women with a family history of breast cancer may benefit more from mammography screenings between ages 40-49 than average-risk women, according to USPSTF.
Watch the task force’s video explaining the draft recommendations.
 Alternate viewpoints
Alternate viewpoints
Dr. Joseph Mercola is an osteopathic physician who’s trained in both traditional and natural medicine. His website, Mercola.com, aims to “transform the traditional medical paradigm in the United States,” and supports his belief that a person’s body has the “unique ability to heal itself and maintain wellness.” Earlier this month, Mercola wrote an article highlighting what he sees as potential harms caused by mammograms and cited several new studies refuting the value of those tests.
He is not without opponents. In a March 2015 article posted on nymag.com, reporter Melissa Dahl writes, "Dr. Joseph Mercola ... is widely considered to be a quack, and [his] health 'advice' has been the target of several warning letters from the U.S. Food and Drug Administration."
We asked Dr. Mercola, a Chicago native now based in the suburbs, to share his thoughts on the new mammogram guidelines from the U.S. Preventive Services Task Force and American Cancer Society and their potential harms, as well as preventive steps he thinks women can take to lower their risk of breast cancer.
What do you think about the new guidelines for mammogram screenings?
I think it’s a move in the right direction. I think it could be more aggressive. I’m not a fan of mammography. There are more downsides than benefits.
What do you see as some of the potential harms of mammograms?
First of all, nearly 40 million women in America are getting mammograms every year. There’s a massive industry built around them and vested interests in perpetuating these guidelines. It’s remarkable these revisions reduce mammograms in light of those vested interests.
Over their lifetimes, one in eight women will receive a breast cancer diagnosis; four of the eight will have one false-positive in mammography within one decade. That puts them down a path where they’re led to biopsies and therapies that could harm them.
Mammograms use ionizing radiation which can increase the risk of cancer. Mammograms are not benign things. It’s not just to say negative comments on mammograms. I’m a big believer in prevention, and the intention of mammograms is good. One should identify cancer before it occurs to implement early therapy and focus more on prevention.
Mammograms do not prevent cancer. I think women are confused and think that it does. There are so many simple interventions that can reduce a women’s risk of breast cancer. My strategy is to encourage a behavior that not only reduces the risk of breast cancer but all [cancers].
What are some of the preventive steps you believe that women can take?
The simplest one—not only to reduce breast cancer but many other cancers and common causes of disease like heart disease and stroke, even neurodegenerative diseases like Alzheimer’s—is to optimize your vitamin D, ideally with sunshine. But that’s not going to work too well now (supplements can be taken). One needs 40-60 nanograms of vitamin D.
One cause of any cancer is insulin resistance. One of the most significant interventions you can do to reduce insulin resistance is to do intermittent fasting, which is not eating food around the clock and going 10, 12, 16 hours without food. The best way to do that is to skip dinner—gradually progress to that level.
Reduce your intake of processed food and sugar. Eat real foods. Exercise. It can be as simple as walking at least 30 minutes to 1-2 hours a day. Multiple studies have shown a reduced risk of cancer and improved longevity.
Limit alcohol, and be really cautious of synthetic hormone replacement: estrogen, synthetic estrogen derivatives in hormone replacements (such as birth control). It’s been well documented with an increased risk in cancer. On the other side, avoid toxins like xenoestrogens—those are synthetic chemicals that mimic estrogen and have been linked to increased risk of cancer on the breast. BPA in plastics are another common toxin. Use glass containers when cooking or storing food.
How important is the emphasis on age in terms of screening, in your opinion?
Of course, the increase in the age you’re recommended to get [a mammogram]—it’s now 45—and then decrease in frequency of mammograms in older women is a move in the right direction.
There’s significant consensus with the medical community showing studies, including one earlier this year in JAMA [The Journal of the American Medical Association], that mammography screenings led to unnecessary screenings and virtually had no impact on deaths from breast cancer. We’re finding more of these studies that show mammograms don’t provide the benefits it’s purported to.
What are alternative tests or tools that you believe could be used to screen for breast cancer, rather than mammography?
There’s breast self-exam, which you have to be instructed properly on how to do. Ultrasound is another one. There’s a tool, thermography, which measures heat signatures. Cancers have increased number of cells in metabolic activity, so they’re warmer and can show up. You do an initial baseline screening, and then once that’s done, do it again and you can see different heat patterns. It’s not diagnostic. You need to also have conventional tests like ultrasound or MRI if there’s a concern or history of breast cancer.
Interview has been condensed and edited.