Health
How Long Should You Isolate If You’re Fully Vaccinated But Have COVID-19? There is Some Debate
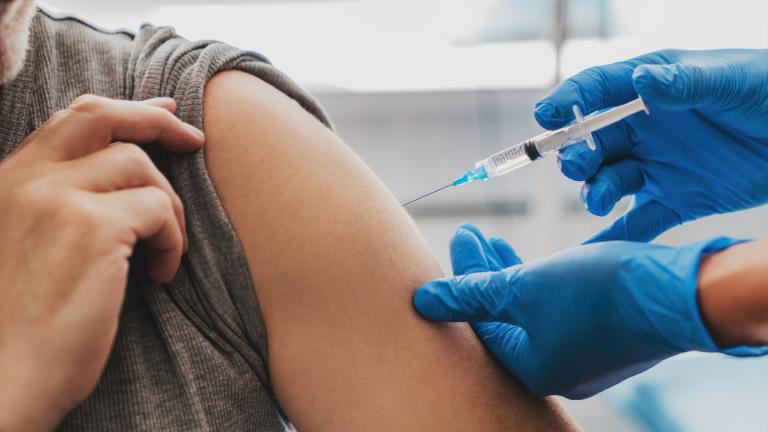
 Health officials warn that more people are expected to get infected with the omicron and delta coronavirus variants and they need to stay home and isolate themselves so they don't spread the virus to others. (David Paul Morris / Bloomberg via Getty Images)
Health officials warn that more people are expected to get infected with the omicron and delta coronavirus variants and they need to stay home and isolate themselves so they don't spread the virus to others. (David Paul Morris / Bloomberg via Getty Images)
(CNN) – As the highly transmissible omicron and delta coronavirus variants continue to sweep across the United States, health officials warn that more people are expected to get infected – even those who are fully vaccinated – and they need to stay home and isolate themselves so they don’t spread the virus to others.
Anyone who has COVID-19 should isolate for 10 full days, according to current guidance from the U.S. Centers for Disease Control and Prevention.
But this holiday season, there has been growing debate around the number of days to isolate if you test positive for COVID-19 but don’t have symptoms and are fully vaccinated – or, better yet, got a booster dose.
This debate comes as COVID-19 cases rise across the United States. As of Tuesday, the nation is averaging 139,764 new cases each day, according to data from Johns Hopkins University – up 16% from a week ago.
“We should have as short of a time period needed for isolation as possible for a number of reasons,” Dr. Leana Wen, a CNN medical analyst and former Baltimore City health commissioner, told CNN’s Kate Bolduan on Tuesday.
“One is for health care workers who test positive. You don’t want those individuals to have to be out of the workforce and then we have a serious shortage. The second reason is, we want to actually incentivize people to find out that they’re positive,” Wen said. “What if you don’t want to miss days from work? You might end up just not testing, because you don’t want to find out that you’re positive. And so, if cutting 10 days to five days – even if we end up missing some percentage of people who may still be infectious – you may actually get higher compliance if you get to a lower number of days needed for isolation.”
Vaccinated people are less likely than unvaccinated to spread the coronavirus to others, according to the CDC: “Vaccinated people can still become infected and have the potential to spread the virus to others, although at much lower rates than unvaccinated people.”
US officials consider shortening isolation time
The CDC now notes on its website that isolation should start the first day you notice symptoms, with day one of isolation being the first full day after symptoms began.
If you test positive for COVID-19 but never have symptoms, day one of isolation is the first full day after your positive test. However, “if you develop symptoms after testing positive, your 10-day isolation period must start over,” and day one is the first full day after your symptoms developed.
But shortening that recommended isolation time is under consideration for those who are fully vaccinated or even boosted – particularly health care workers, Dr. Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases, told CNN’s John Berman on Tuesday.
“That’s certainly an important consideration, which is being discussed right now,” Fauci said.
“For example, if you get a health care worker who’s infected and without any symptoms at all, you don’t want to keep that person out of work too very long,” he said, especially if those personnel are needed due to a rise in illness this winter and hospitals possibly running out of beds.
“If you do have someone who’s infected, rather than keeping them out for seven to 10 days, if they are without symptoms, put an N-95 mask on them, make sure they have the proper PPE, and they might be able to get back to work sooner,” Fauci said.
The United Kingdom is one nation that has shortened the self-isolation period. The U.K. Health Security Agency announced that beginning Wednesday, the self-isolation period for anyone with COVID-19 is reduced from 10 days to seven days, if the person has two negative lateral flow test results taken 24 hours apart. The first test should not be taken before the sixth day.
Many physicians and scientists pose that if someone is fully vaccinated, they can test themselves to determine when they no longer need to isolate.
“I think that fully vaccinated people should be able to use rapid tests to guide them regarding the length of their isolation period,” Dr. Amesh Adalja, a senior scholar at the Johns Hopkins Center for Health Security, wrote in an email to CNN on Monday.
“I think we should be using rapid tests to shorten isolation periods – people should be able to end isolation when they are negative on a rapid test as they are no longer contagious,” Adalja wrote. “Quarantine periods can also be modified by using serial antigen testing to know one’s status and allow for safe interaction. Omicron makes this a more pressing concern as infection and exposure are going to become much more common.”
Quarantine refers to when someone has been exposed to the coronavirus that causes COVID-19, may or may not have been infected, and therefore needs to avoid others. Fully vaccinated people do not need to quarantine unless they have symptoms, according to the CDC.
Isolation, by contrast, is when someone tests positive for COVID-19 and needs to isolate from others until they are no longer contagious, even if they don’t have symptoms.
How to tell if your symptoms are COVID or something else
Testing for COVID-19 is key, as it can be hard in some cases to tell COVID-19 symptoms from the flu or even the common cold.
Dr. Christina Johns, a pediatrician in Annapolis, Maryland, told CNN this month that there has been a “slow but steady” increase in patients testing positive for flu and COVID-19 in her pediatric network in recent weeks.
This winter, there is concern over a potential “twindemic” of COVID-19 and flu, and it’s important for people with any respiratory symptoms this season to see their doctor immediately for testing, said Johns, an emergency medicine physician and senior medical adviser for PM Pediatrics, which has more than 70 pediatric office locations across the United States.
She said that when young people – up to age 26 – come into her office with symptoms, such as a cough, fever or runny nose, the only way to determine whether they have the flu, COVID-19 or a common cold is through testing.
“I think that that’s an important point that needs to be made, especially right now while we are still in the midst of this pandemic,” Johns said.
“It is difficult to tell the difference without a test. There are some trends. Typically for influenza, the clinical hallmark is high fever, and that occurs less so in the common cold and is not always a feature of COVID-19 infection,” Johns said. “But none of that is 100%, and there’s enough overlap in all three of these that, really, the only way to know the difference is through testing.”
The-CNN-Wire
™ & © 2021 Cable News Network, Inc., a WarnerMedia Company. All rights reserved.