Health
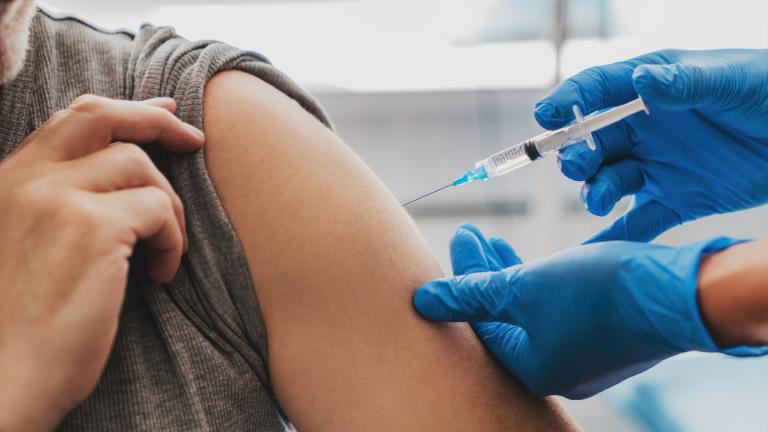
How Health Care Providers Are Preparing for COVID-19 Peak in Illinois
The Chicago Medical Society, an organization that represents more than 17,000 doctors, says that as of Monday, intensive care units in Chicago are full.
“We are at capacity in the ICU in the city of Chicago at this time,” said Dr. Jay Chauhan, president of the society.
Illinois now has 5,057 reported cases of COVID-19. With limited testing, however, the number is assumed to be low. There are hundreds of new cases reported a day, and Illinois now has 73 deaths associated with the new coronavirus.
Experts say the number of cases in Illinois will peak within two to three weeks.
At the University of Illinois Hospital, 18 nurses have so far tested positive for COVID-19, according to Alice Johnson, executive director of the Illinois Nurses Association. Future staffing as more health care providers test positive is just one of her major concerns.
“There is no limit on the number of patients that a nurse can be assigned (to), which means that a lot of hospitals stretch their nursing staff,” said Johnson. “There aren’t enough nurses working there to begin with. Now we’re in a situation where nurses are starting to become sick and we’re looking at stretching that staff even further.
“The intensive care unit nurses are highly skilled and experienced. They’ve been working on those units for a long time and we have concerns about safety if the staff who have the experience on those units get sick and are no longer able to work them. You can’t just take any nurse and put them on an ICU unit. It’s not safe,” Johnson said.
So how are health care providers and hospitals on the front lines dealing with the crush of patients? And what are hospitals doing to prepare for the weeks ahead?
“Hospitals are preparing daily and really around the clock for the coming wave,” said A.J. Wilhelmi, president and CEO of the Illinois Health and Hospital Association, which represents more than 200 hospitals and health systems across the state. “It is paramount for us to keep our health care workers safe and protected. And so we have been working as a hospital community with our government partners and others in the supply chain to get access to personal protective equipment and to make sure that we have the supplies we need to keep our workers safe.
“We’re also looking at a surge capacity within our current existing hospitals. We know that the governor and the mayor are looking at standing up a field hospital at McCormick Place for up to 3,000 beds, all that activity in coordination between the hospital community and our government partners is going to be critically important as these days continue to evolve and we see the numbers increase,” Wilhelmi said.
According to a recent survey of the physician members of the Chicago Medical Society, one-third of the 900 doctors who replied believe they have been exposed to the COVID-19. And 85% of emergency medicine doctors surveyed say they have been exposed to the coronavirus.
“We’re hearing from the doctors who are an emergency room and in the ICU is it’s kind of like a war zone,” said Chauhan. “Within a 30-minute period at one of the major medical centers in Chicago, they had to intubate five COVID-19 positive patients … which is pretty remarkable. So there’s five ventilators, five ICU beds being immediately taken up.
“There’s a big, big, big concern about personal protective equipment not only from a personal standpoint, but you certainly don’t want to see an asymptomatic individual who comes in to be evaluated and then carry that disease to your next patient,” Chauhan said. “So, it’s not just for self-protection but also protection for our future patients. So if we’re ill and unable to go to work or if we communicate the disease to other individuals that would create a lot of harm.”
Gov. J.B. Pritzker made a plea last week for retired medical providers to help during the crisis. But people who are 60 years old and older have a greater risk of contracting the coronavirus.
“We’re going to make sure that we use every precaution necessary to keep our workforce safe and protected,” said Wilhelmi. “Those retired individuals will have to make a decision for themselves and what’s best for them and their families. But at the same time we are hearing from retired health care professionals. They understand the urgent need and they want to be helpful. And I think that decision will be made on an individualized basis.
“We’re not at peak. We have enough providers today, but we need to make sure that we’re doing everything we can to, number one, keep our health care workers safe and protected,” Wilhelmi said.
But the nurses say there’s currently not enough personal protective equipment (PPE) to ensure the health and safety of any front-line health care providers.
“It’s one thing to ask a nurse to return to work in a potentially high-risk situation because we know that there’s health care workers out there and nurses out there that have become infected even with all of the proper PPE,” said Johnson. “But what we’re talking about here is situations where nurses are lacking PPE and then we’re asking for a retired nurse who is potentially older, potentially already has more health problems, and have them come into a situation that is already not made as safe as it could be with the lack of equipment.”