Health
Who, What and How? The Challenge—and Confusion—of Coronavirus Testing
Gov. J.B. Pritkzer on Wednesday declared the availability of testing for the new coronavirus – or the lack thereof – to be the greatest challenge Illinois has faced in combatting the outbreak.
But he’s hopeful that will soon change.
Abbott on Wednesday announced that it has Food and Drug Administration authorization for its COVID-19 molecular test, and will begin to immediately ship 150,000 kits to U.S. customers.
And increasingly, hospitals’ in-house tests are coming online.
On Friday, NorthShore University HealthSystem announced that it went live with its novel coronavirus test.
“One of the reasons that we did this is because 10 years ago when we were faced with the swine flu epidemic, we found ourselves in a situation to offer testing there,” said Dr. Karen Kaul, who chairs NorthShore’s pathology and laboratory department, according to a transcript of a conference call Friday. “Right now we are looking at ways to increase the capacity of our testing here at NorthShore so that we can test more patients, because I expect demand will go up.”
Advocate Aurora Health is also on the precipice of processing its own COVID-19 tests.
“ACL Laboratories, which is part of Advocate Aurora Health, is in the process of finishing testing validation and training for COVID-19 testing. Once operational, ACL Laboratories will be able to perform at least 400 tests daily with results back in fewer than 24 hours,” according to a statement.
Both NorthShore and Advocate say those tests will only be available to doctor-authorized patients, such as those who have flu-like symptoms but who test negative for influenza or other common respiratory illnesses, or who traveled from affected places like China and Italy.
“These are not drive-up windows like you’re going to a fast food restaurant,” Dr. Robert Citronberg, an infectious disease doctor with Advocate Health Care, said on a Wednesday media conference call. “They’re not open or available to the general public."
Additional drive-through sites are in the construction phase.
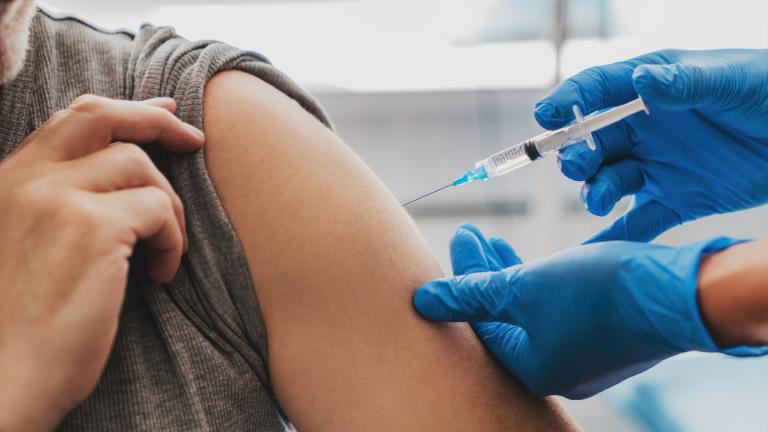
The test itself will involve a swab of the throat or nose.
Sarah Connolly, a DePaul university microbiology professor, studies herpes viruses – which, like the coronavirus – is detected using a type of test called a “PCR test,” short for polymerase chain reaction.
Here’s how it works, as she explained it: After a medical professional swabs your nose or throat, the sample is sent to a lab which extracts the genetic information, the RNA (ribonucleic acid), which is then copied into DNA “because DNA is easier to handle.”
That’s when the PCR steps begin.
“You’re able to replicate the DNA. And that’s what we’re asking in the PCR test: Is there DNA present in the sample that came from coronavirus?” Connolly said.
To do that, a lab uses tiny pieces of DNA called primers, which are specific for a target, “so these primers for coronavirus, they’re going to bind to coronavirus and only to coronavirus.”
“So in the PCR test you have your sample, you add your primers, you run the test and if those primers bind to the coronavirus DNA, it will cause, in the reaction you’ll get a replication of that DNA,” Connolly said. “So if you had a sample that did have coronavirus DNA in it, now you’ll be able to see that coronavirus DNA. On the other side, if you have a sample that doesn’t have any coronavirus DNA in it, those primers have nothing to bind to so they won’t replicate any DNA and you won’t see the presence of any DNA from the coronavirus.”
It works the same for other viruses; different primers are used for the specific pathogens, whether it’s for the coronavirus, HIV or hepatitis.
While it isn’t a test that can be done at home, the methodology’s common.
“It doesn’t require very high-tech equipment,” Connolly said. “Most universities and hospitals have the equipment that they would need to be able to run this PCR test. What you need to be concerned about is safety with those samples. So a random lab can’t just run this test. They have to have the safety protocols in place if they’re handling samples that potentially are contaminated with coronavirus.”
Pritzker, who blames the federal government for rejecting a World Health Organization test in favor of U.S.-made ones – despite the country’s supply chain not being prepared – says it’s important that Illinois get more tests so more sentinel surveillance can be done.
“In other words being able to see where the outbreaks are taking place across the state,” he said. “Being able to separate people who test positive and are in a community of vulnerable people. That’s a very important thing to do. If you don’t have tests you don’t know where to go to make those adjustments. That’s what’s happened.”
Pritzker said he has tried to get ahold of necessary test supplies, but they’ve “mostly been monopolized by the federal government and delayed in their distribution. And so I’m trying to essentially grab whatever part of the supply chain I can for the state of Illinois.”
Pritkzer said businesses have been willing, and in recent days have gotten supplies to Illinois that will increase the state’s testing capability.
“We’ll be able to do more tests. It’s still not enough,” he said. “You talk about thousands of tests? We need to be able to test many more people than that.”
The limitation on tests makes it difficult to know how many actual cases of the coronavirus there are; Illinois’ confirmed cases have been rising – up to 288 on Wednesday – but that’s only a percentage of the true number, given how many individuals may have the virus but will not be tested for it, especially given that the vast majority of COVID-19 cases are mild. Health officials are begging anyone who can weather their illness at home, the so-called “worried well,” to do so rather than taxing a health care system they want to preserve for only the most acute and life-or-death cases.
But Connolly says it’s likely that once medical experts get a better handle on testing for COVID-19 – and treating it – attention will be turned to creating a different type of test that will look for the presence of antibodies.
“The presence of an antibody against a specific pathogen says that you are exposed to it at some point in the past,” she said. “So I think after this outbreak is contained, we may start doing that type of testing to find out who was exposed and to get a real answer to that denominator. Like, how many people did get infected with this virus?”
Pritkzer says Illinois needs more tests.
Follow Amanda Vinicky on Twitter: @AmandaVinicky